The Bryn Mawr Urology Group - A Division of Academic Urology | 919 Conestoga Road Rosemont, Pa 19010
DaVinci Robot Experts
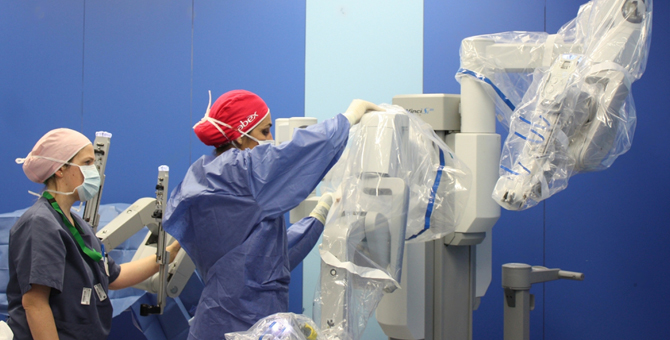
Advanced robotic surgery for prostate and testicular cancer at Bryn Mawr Urology

Bryn Mawr Urology specializes in the world’s most state-of-the-art treatments of prostate cancer surgery, utilizing the da Vinci robotic surgical system which facilitates Laparoscopic Prostatectomy. Expert Urologic Surgeon Dr. David McGinnis, M.D. received his bachelors degree, cum laude, from Harvard College, Cambridge, Massachusetts and his medical degree from the University of Texas Health Science Center at San Antonio, Texas. He studied laparoscopic radical prostatectomy with the Originators of Laparoscopic Prostate Surgery at the Institute Mutualiste Montsouris in Paris, France with Drs. Guy Vallancien and Bertrand Guillonneau. Dr. McGinnis served both his general surgery and urology residencies at Thomas Jefferson University Hospital, in Philadelphia, Pennsylvania.
He is among the first urologists to implement this procedure in the United States and was among the first urologists to perform laparoscopic radical prostatectomy in Pennsylvania.
Meet the experts in da Vinci robotic surgical system at Bryn Mawr Urology
Dr. David McGinnis, M.D. and the Bryn Mawr Hospital O.R. team successfully completed the first prostatectomy done at Bryn Mawr using the da Vinci® robotic surgical system on Monday, July 10, 2006. The patient, age 60, was diagnosed with prostate cancer and required a radical prostatectomy (or removal of the prostate gland). While this was Dr. McGinnis’s first robotic prostatectomy at Bryn Mawr Hospital, he is, in fact, one of the most experienced in the region in this procedure.
Expert Urologic Surgeon Dr. Ilia S. Zeltser, M.D. at Bryn Mawr Hospital, is among an elite group of physicians nationwide and the only in the Philadelphia region performing laparoscopic Retroperitoneal Lymph Node Dissection, a safe and effective way to treat testicular cancer, as well as help establish its exact stage and type, with less pain and faster recovery when compared to traditional surgical procedures. Dr. Zeltser has extensive experience in both purely laparoscopic and robotically assisted laparoscopic prostatectomy. Dr. Zeltser completed one of the most prestigious fellowships in minimally invasive and robotic surgery, and served as an Instructor of Urology at University of Texas Medical Center. Dr. Zeltser and colleagues reported the first ever single port scarless laparoscopic kidney removal. Dr. Zeltser has published over 20 original articles along with numerous abstracts, book chapters and editorials in minimally invasive surgery and currently serves as a Clinical Assistant Professor of Urology at Thomas Jefferson University.
Single Keyhole Incision Revolutionizes Kidney Surgery at Bryn Mawr Hospital
Ilia S. Zeltser, MD, Urologic Surgeon at Bryn Mawr Hospital, is among a small group of urologic surgeons worldwide and the first in the Philadelphia region to remove part of a patient’s diseased kidney through just one tiny incision hidden in the belly button. This less invasive approach has the potential for faster recovery, less pain, and improved cosmetic outcomes.
“This innovative technique takes traditional laparoscopic kidney surgery to the next level and leaves patients with a barely noticeable scar tucked away in the navel,” said Dr. Zeltser, who was among the physician team of researchers at The University of Texas—Southwestern Medical Center to develop the single-keyhole approach for kidney surgery a few years earlier.
Conventional laparoscopic surgery typically requires the insertion of a tiny video camera and several thin instruments through a few small incisions. However, Single Port Access (SPATM) surgery, also known as Single Incision Laparoscopic Surgery (SILSTM), One Port Umbilical Surgery (OPUS), or Natural Orifice TransUmbilical Surgery (NOTUS), is a procedure in which the surgeon operates almost exclusively through a single entry point, typically the patient’s naval.
2014 Dr. David McGinnis, MD Voted Top Docs Philadelphia Magazine
David McGinnis, MD, a Bryn Mawr Hospital urologist, is among the first in the Philadelphia region to remove cancer from the prostate through a minimally invasive procedure called laparoscopic radical prostatectomy.
Faster recovery and less pain with Bryn Mawr Urology’s innovative prostate cancer surgery
Only a few centers nationwide are currently performing this procedure. For patients undergoing laparoscopic procedures, there is less pain and quicker recovery than following conventional surgery. Kidney cancer tends to affect both men and women almost equally and tends to affect people in their 40’s to 80’s with the greatest incidence affecting people in their 60’s. Minimally invasive surgery can remove a cancerous kidney just as effectively as traditional open surgery while giving adults, children and infants patients the same long-term survival. The symptoms of kidney cancer typically are a pain in the flank or upper side of your back that doesn’t go away, a feeling of poor health, blood in the urine and in some cases, a mass you can feel in the flank.
NEW: Patients will have three small incisions in their side below their ribs for the procedure. The procedure generally takes just between three and four hours and the patient can expect to have a hospital stay of one to two days.
OLD: The old way might find four half-inch incisions in the abdomen, along with one three inch incision near the navel rather than the conventional, 12- to 14-inch incision. A laparoscope is inserted, allowing surgeons to extract the kidney without having to remove part of a rib or make the very large, tissue-cutting incision required with the surgery in the past. As a result, donors can leave the hospital in three days and return to work in about 16 days.
The future of surgery is here: Bryn Mawr Urology’s da Vinci robotic surgical system
In the article “Showing How Hospitals Operate Main Line School Night will introduce medical experts and equipment to students – stress-free”, The Philly Inquirer Sun, Sep. 16, 2007, Bonnie L. Cook writes:
“No doubt about it, getting wheeled into an operating room is a frightening prospect,” said Bryn Mawr Hospital’s David McGinnis, a urologic surgeon. But help is on the way: a new “mini medical school” for adults being offered by Main Line School Night in tandem with Main Line Health. The series is designed to give students informal time with medical experts, such as McGinnis, whom they might not otherwise get to know. It also gives them a rare view behind the scenes at a major hospital.
Mini medical school was the brainchild of Michelle Stewart, Bryn Mawr Hospital’s communications and marketing manager. She had attended a series of science classes at the night school and thought a similar series based on patient care might be interesting. Stewart’s course proposal consisted of lessons built around six subjects: the body, managing health, diagnostic tools, medicines, surgery, and the business of running a hospital.
For McGinnis, who specializes in removal of cancerous prostate glands using a robotic device, the decision to take part was a no-brainer. “Education is a lot of what I do with patients so they understand the technology that comes to bear on the situation,” McGinnis said. “It’s all of a piece.” He and patient-care manager Lynne McGrath will conduct a tour of the operating room, where the hulking robotic device sits. She’ll talk about measures the staff takes against infection and errors. They will have one student lie on the operating table. McGinnis will demonstrate how he looks through the robot’s viewer, and conducts the procedure without putting handheld instruments on the patient. “This machine works by virtual reality,” he said. “It feels like I’m inside the body.” As McGinnis maneuvers the controls with hands and feet, the computer inside the robot takes his commands and scales them down to the size of the operation. “It’s like playing the organ,” McGinnis said. The surgeon plans to let pupils sit down and look through the viewer. When people put their hands on a device and see how it works, they lose their fear, he and McGrath said. “Why not have fun with the gee-whiz factor of this nifty tool? It’s neat technology,” McGinnis said. See the Robot in Action – This video shows the beauty and genius of the technology.
Bryn Mawr Urology now brings the da Vinci robotic surgical system which performs remote telerobotic surgery.
Experience the highest quality of care for prostate and testicular cancer at Bryn Mawr Urology
The da Vinci system consists of three components:
- a surgeon console with an integrated three-dimensional display stereo viewer
- a robotic manipulator with three cart-mounted arms (one arm for the camera, two arms for the 8 mm instruments)
- vision cart
Visualization is obtained by two three chip cameras mounted within one integrated, three-dimensional 12 mm stereo endoscope with two separate optical channels. The laparoscope is controlled by moving the master robotic handles. The operative images are transmitted to a high resolution binocular display at the surgeon console. Unique laparoscopic instrument tips, called “Endo wrist instruments”, provide articulated motion with a full seven degrees of freedom inside the abdominal cavity. Tip articular mimic the up/down (“PITCH”) and the side-to-side (“YAW”) flexibility of the human wrist. Instrument tips are aligned with the instrument controllers electronically to provide optimal hand-eye orientation and natural operative capability.
Dr. Mcginnis said, “A current standard treatment for prostate cancer is radical prostatectomy, in which an eight-inch incision is made in the patient’s lower abdomen to remove the prostate. “The clear advantages of performing this procedure laparoscopically are decreased pain, quicker recovery and less bleeding,” he explained. “The future of surgery is to become less invasive and limit the side-effects of treatment, and this is a big step in that direction.”
Dr. McGinnis said patients who would not be good candidates for the minimally invasive procedure are those with prior prostate cancer treatment, including hormonal therapy and radiation therapy, and obese patients. After lung cancer, prostate cancer is the second leading cause of cancer death among men in the United States. On an annual basis approximately 45,000 surgical procedures are performed to remove the cancerous prostate.
Robot History
AESOP robotic arm was first surgical robot approved by the US Food and Drug Administration, but is no longer used.
PR Newswire, Sept 17, 2002 BRYN MAWR, Pa. — Bryn Mawr Hospital surgeon David McGinnis, MD, is changing the way prostate cancer is being treated, using a AESOP. Dr. McGinnis is among the first urologists in the United States to use robotic technology to enhance his minimally invasive surgical techniques, however AESOP is no longer used by Dr. McGinnis for Prostrate Cancer Surgery [PDF]

